Long ago as a senior emergency doctor in New Zealand I was defibrillating hearts, reading ECGs, relocating dislocated shoulders, resuscitating shocked patients… Full-on! But kinda straightforwardly full-on. Nearly all problems had a right answer, validated with case controlled trials. We needed clinical skills to diagnose ("Ah this is meningitis") plus knowledge and technical skills to implement those right answers (="Ok Lumbar puncture then ceftriaxone 1 gram iv"). Mostly we got it "right" (=best practise). Occasional complicated cases- say a pregnant 27 year old with a history of asthma, a fractured femur from a car accident and a concomitant kidney infection- needed many consultant heads together. Hmmm. There’s no clear best practice, but despite differing opinions on exactly what to do or in what order even here we'd agree on the major issues and a general approach. Our aim was still well validated good practice.
Christchurch Emergency Department, New Zealand- not! Welcome to Rio Sucio... The bullet holed sign avers that, with our help, the government will defeat guerillas and drug traffickers.
ZImmerman Stacey matrix: y-axis= agreement on the problem, x- axis = certainty about the solution. The blue zone is complexity.
The next year my wife Kaaren (also a dreamy doctor) and I found ourselves leading an MSF programme in Uraba, Colombia where swamps, mosquitos and FARC guerillas stop the the Pan American highway dead in its Alaska-to-Chile tracks. Without roads we wove our uncertain way up muddy waterways. There we were, amidst jungles, flooding rivers, non-Spanish speaking indigenous people, displaced black people, left wing guerillas, right wing paramilitaries, a nervous army, anopheles mosquitos, malaria parasites, gold prospectors, bandits, a disengaged government... once a jaguar leaped into the water beside our canoe, so close I could smell it. Surreal! Without a blueprint and with no source of evidence for the best, or even a good, health programme we were up a creek without a paddle.
What's the problem? Without epidemiology to tell us what the health issues were what should we aim for? We picked malaria, based on anecdotal rather than formal evidence but equally justifiably could have chosen child mortality, leishmaniasis or many other things. OK, were going to 'do' malaria, now what? No evidence based randomised double-blind study defines what to do or how to tackle malaria in a war in Uraba. A ’wicked’ problem. Stacey's matrix (modified by Zimmerman) plots problems on two axes- certainty about the problem and degree of agreement on the solution. By that definition we were on the far side of complexity, verging into chaos, far distant from the knowable safety of New Zealand medicine. Best, even good practice now? I didn’t have a clue.
But Mario did. Our country medical coordinator fresh from a MSF "med-co" course, led a team retreat. With his guidance we defined and categorised the issues and produced a beautiful logical framework. Even the guerillas found a place in the risks and assumptions column. Aaah! Development was reducible, ordered and plan-able after all. Just like medicine! It felt good.
Definitely in a different space now. Teaching health workers parasitology- My only medical job were gumboots were work uniform.
An indigenous boy (unhappily) gives our health workers a drop of his blood for a practice smear.
So began one of the most exciting projects I’ve been involved in. We set up a field office in the ramshackle, flooded jungle town Rio Sucio (literally 'Dirty River', colloquially 'Shit Creek') and worked with everyone from indigenous shamans to government officials. Employing Colombian microbiologists we ran a month long course in malaria diagnosis and treatment. I loved seeing volunteers selected by indigenous and black villages able to take blood films, correctly stain them, diagnose -falciparum or vivax malaria?-and treat appropriately. Those who passed a rigorous end-of-course-exam were presented with a box of medicines and one of the mirror microscopes we’d argued out of the government. We’d even arranged quality control (slides and diagnoses sent down-river in canoes, reviewed and sent back up with pathologist's opinion) and a maintenance schedule with the local hospital. We had buy in from shamans and voodoo healers and even taught communities about permethrin impregnated nets and how to identify and destroy mosquito breeding sites. It was a wonderful programme, totally captivating for an erstwhile kiwi emergency doctor. Everything was covered. Logically framed one might say.
Our malaria workers examine a practice slide. A passing soldier wouldn't miss the fun
One morning our country office phone rang. The caller noted our good work but, pointing out "Uraba could be risky for your health”, suggested it was best we left. This was a death threat, the health risk being acute AK-47 induced lead poisoning. Head office instructed us to get out, pronto. We left the next day. The day after that a flotilla of paramilitaries went up river, "undetected" by Rio Sucio government troops and killed many including some of our community workers. Meanwhile tails between legs Kaaren and I were on a Bogota-Amsterndam flight. While we debriefed in the MSF Holland head office two of our community workers were held hostage by a paramilutary faction somewhere in the Uraba backwaters and mould had started its inexorable creep over our microscopes in the jungle.
Faliciparum malaria still rules Uraba.
Community extension: With palm frond wings I role play a mosquito in an Embera village
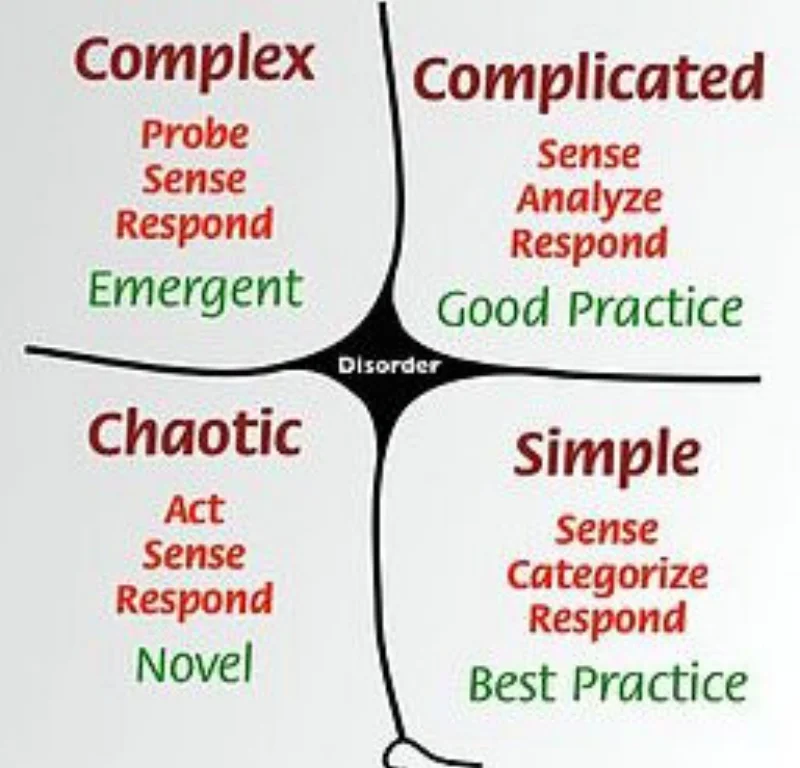
In the 17 years since I have reflected a lot on that first foray into international health, wondering what happened and why. More useful for me than Zimmerman's matrix is Snowden’s Cynefin framework breaking the world into different spaces- domains- each needing different thinking and logic. We got the 'domain' -and the logic- wrong.
Thinking like doctors we treated a malaria project with indigenous and displaced black people amidst flooding tropical rivers in a war zone in Colombia like any other medical problem. Complicated sure, but soluble with science, rationality and anti-malarials. We defined good practice and packaged it in a logical framework. Inside our boundaries was stuff we could deal with. We excluded the rest, just deposited it in the too hard basket (aka "risks and assumptions" in a log-frame). The photos to the right show us working in our boundaries:- starting with science we involved people and tried to impart appropriate knowledge. All well planned and thought out. We were thinking and acting the wrong way, using logic not valid for the complex, possibly chaotic space we were in (most of development is). Where we should have been "trying to facilitate the emergence of beneficial coherence" (Snowden) we simply rationally planned and implemented... Our workers were killed and our project "failed". So it goes.
~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~
So What?
Over the years since Kaaren and I left Colombia, the years since paramilitaries killed Macario, the years in which I have moved from a rational Emergency doctor into more intuitive development thinking I've thought and re-thought this experience. Here are some of my questions:
Snowden's Cynefin with heuristics on how to operate in each zone.
Zimmerman’s matrix, continuous on both axes, has fuzzy borders between areas. Snowden has discreet domains defined by the relationship between cause and effect. In each qualitatively different thinking applies. For me Snowden's analysis is more useful practically. A big take home for him (and me) is that an essential development skill is to recognise domains and be able to switch thinking and operational style to match the space you’re in. What do you think? Can different parts of projects really work differently? Do we really have to continuously switch thinking, even change methods and what we're aiming for? Is OM particularly relevant to some domains?
See Snowden explain Cynefin here.
Bob Williams (and others) see relationships, perspectives and boundaries as critical to complex systems. Relationships and perspectives yes, but a priori judgments of value or worth or what’s in and what’s out don’t work for me. By definition complex systems are open, un-bounded. The boundaries we drew had us, indigenous, displaced black people and guerillas in. The paramilitaries were left out. They did not see it that way.This was their space too. OM by deliberately working with boundary partners, forces us to look at the world through others' eyes, thus preventing us imposing our values and boundary decisions on the systems we work in. I like that. What do you think? (For Williams' views on systems see here: http://www.bobwilliams.co.nz/Systems_Resources.html)
An outcome mapping approach to this situation would have focused on human actors in the system more than plasmodia, microscopes diagnostic skills and anti-malarial pharmacology. At the time we could not see that the system may have been chaotic ( even retrospectively its unclear why the paramilitaries threatened us and killed our workers). In this chaos would OM really have been better than the much maligned logical framework?
A security call with satellite phone. The flag is for the guerrillas, on the tangled bank, certainly watching. We never thought to ask what the paramilitaries were thinking. They hadn't emerged yet. .
Complexity demands emergent rather than predefined practice. Here, although it was illegal to work with “actores armados” we’d contacted guerilla leaders and requested they let us work in 'their area'. They agreed, stipulating we always fly our flag. At the time we did not realise that even though it was a left wing guerilla area, we also needed right-wing paramilitary buy-in. In truly complex and even more in chaotic systems (development always entails complexity and some chaos) it is often hard to predict who relevant boundary partners are until they emerge- as the paramilitaries did. In fact the system itself , evolving as a project runs, is emergent. So picking boundary partners at the start and defining outcome challenges and progress markers is problematic. How should we plan and implement in evolving systems?
I wrote this as a discussion piece for the Outcome Mapping Learning Community. If you would like to comment please go to to the OMLC website www.outcomemapping.ca and add your two cents. The discussion itself is at http://www.outcomemapping.ca/forum/viewtopic.php?t=1787 For my brief description of what OM is see: outcome mapping
So what? An indigenous girl in a jungle community still ruled by malaria and war.